Why Retinal Screening Matters
Why Retinal Screening Matters
(This is the first of three short pieces dealing with retinal screening, which can mitigate the risk of diabetic retinopathy)
Retinal screening is a key aspect of diabetes patient care. However, non-attendance at eye clinics has been recognized as an independent risk factor for poor outcomes from diabetic retinopathy (DR).
In this vein, an insightful article from the UK’s ‘Community Eye Health’, courtesy of the International Centre for Eye Health[1], has attracted our attention.
Highlights include:
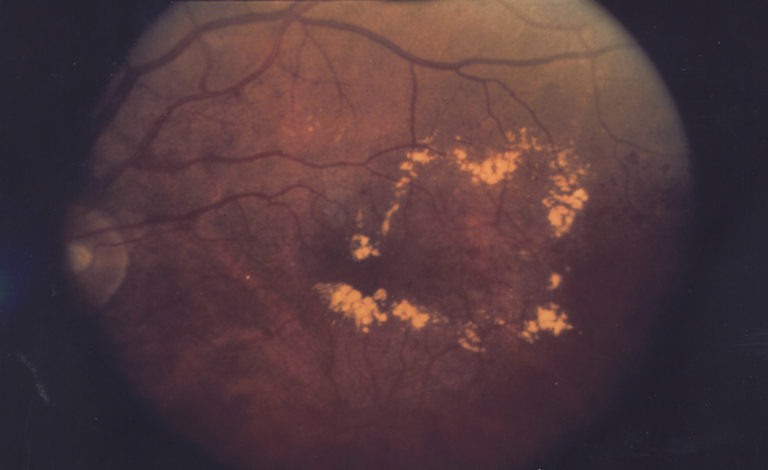
The greatest risk factor for loss of vision due to DR is the failure to attend retinal screening or treatment
Many people with diabetes are unaware that diabetes also affects their eyes and may not understand why screening and early treatment are required.
The UK findings are relevant to people with diabetes, wherever they live. Since the UK provides free basic health care, the cost of treatment is not a barrier there, but it’s likely to be one where patients must pay for eye examinations and laser treatments.
The “eye-opening” (sorry!) study found that while most patients knew that diabetes could affect their eyesight, many were unaware that it could lead to severe visual impairment. This was partly because health workers are reluctant to use the word ‘blindness.’
In addition, patients didn’t realize that they would only experience symptoms once DR had become very advanced, and that treatment would be most effective if given before there were symptoms. Some patients with Type 2 diabetes thought that it was ‘less severe’ than Type 1, and that they were therefore unlikely to experience vision problems; they thought screening was unnecessary.
Patients’ expectations of laser treatment were high, perhaps too hopeful. They were therefore often disappointed in the outcomes; this led to loss of confidence in the health services and skipping appointments. Laser treatment was frequently described as both painful and frightening for patients. Doctors were perceived as unsympathetic, which also made patients less likely to return.
Patients reported that they were afraid of finding out how bad their retinopathy was. Some patients knew that progression of retinopathy is linked to poor blood sugar control. However, many didn’t understand that it’s inevitable to develop some retinopathy after having diabetes for twenty years, no matter how well it’s controlled. When these patients were referred to the eye clinic, they felt that this was because they had failed to control their diabetes, giving rise to feelings of guilt and low self-esteem.
All this underlines that regular retinal examinations are essential for identifying DR and applying timely laser treatment before significant vision is lost.
There’s lots of food for thought here. And some good reasons to see why the Retina Risk App can help to contain this growing epidemic. The app is a unique tool that empowers diabetics to assess in real time their risk for sight-threatening DR, based on their risk profile, and to track the progression of the disease over time. It empowers diabetics to become more involved in their health care decision-making and could significantly lower the risk of potentially blinding diabetic eye disease and expensive interventions.
See our forthcoming blogs on social attitudes and enabling and disabling factors related to DR.